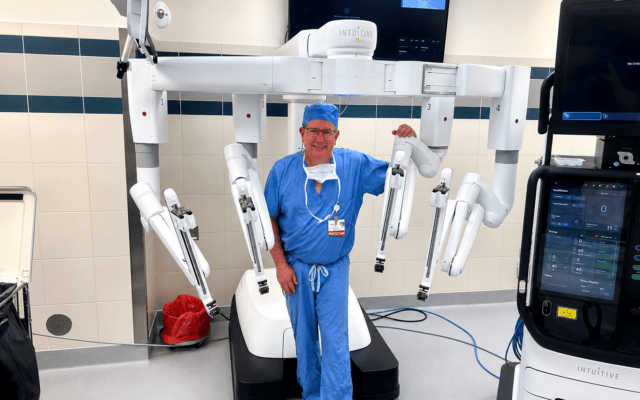
Stryker study bolsters Oaklawn’s Mako robotic-arm technology for joint surgeries
Oaklawn’s joint-replacement patients can expect positive, effective outcomes through the use of robot-assisted technology, based on findings by Kalamazoo-based Stryker Corp.
That’s good news for hip and knee patients of Oaklawn’s Sports Medicine and Orthopedic Surgery team, who’ve been working the past four years with the Mako Robotic-Arm Assisted Technology created by the multinational medical-technologies corporation.
In early 2019, Oaklawn became the first hospital in Calhoun County to offer the system to its patients. Since then, its team of board-certified orthopedic surgeons has continued to gain expertise in applying the technology to patients’ joint issues, including hip and knee replacements.
“Because of this innovative technology, a surgeon is able to personalize the procedure to meet the individual needs of each patient, while improving outcomes,” said Oaklawn orthopedic surgeon Kimberly McLean, D.O.
More than 1,000 Mako SmartRobotics systems have been installed in every state in the contiguous United States as well as 28 other countries, according to a Stryker study based on 15 years of experience with robot-arm assisted surgery.
That study was based on data collected internationally, indicating such systems are in use by more than 100 ambulatory surgical centers as well as more than 48 teaching institutions. In addition to the number of robotic procedures cited in the report, total procedures have surpassed one million, McLean added.
The full report, entitled “The clinical and economic value of Mako SmartRobotics,” may be downloaded online from stryker.com.
The system is described in the report as differing from other robotic platforms in several effective ways. For example, it’s the only robotic-arm assisted surgery system with three-dimensional (3D) planning based on computerized tomography (CT) and AccuStop haptic technology, McLean said.
“The implant position, tracking and soft tissue balancing are assessed in a virtual 3D model by combining a preoperative CT and intraoperative bone registration,” according to the study. “While plain film radiographs (X-rays) provide a 2D image of the scanned area, anatomic structures may overlap, creating an image which is less detailed than a CT scan.”
The CT scan is a vital step in generating a 3D model of the joint, allowing the surgeon to create a detailed surgical plan, she said.
“It means the surgeon knows more than ever before about each patient prior to their surgery and can create a personalized plan based on that patients unique and individual anatomy and condition,” she said. “That’s different from what normally happens in a manual procedure.”
As a result, the Mako Smart Robotics System “has the capability to virtually create and modify the 3D preoperative plan before an incision is made, and the surgeon is able to analyze and modify the preoperative plan before bone resection even begins,” the Stryker study reported.
During the course of surgery, the system is used to modify the surgical plan virtually, and to assist with executing precise bone resections, McLean said. The robotic arm does not automatically perform the surgery, but is used as a tool guided by the surgeon to execute the chosen plan.
“A surgeon using this system also can dynamically balance the knee prior to actually placing the implants, which means they can assess how normal or natural a patient’s knee will feel after the procedure,” McLean added.
“Because of these procedures, patients who undergo joint replacement surgery using this system tend to recover faster, experience less pain and have less blood loss than those who have undergone manual joint replacement surgery,” McLean said. “Such patients also have been proven to have higher satisfaction with the results.”
The Mako Smart Robotics system has demonstrated “higher accuracy and precision to plan for implant placement and sizing for total knee, total hip and partial knee arthroplasty compared to manual techniques,” according to clinical studies cited in the Stryker report.
The system was the first and remains the only robotic technology that can be used across the orthopedic service line to perform total knee, total hip and partial knee procedures, according to Stryker.
“We’re privileged to have tools that we consider state of the art at a hospital the size of Oaklawn,” added orthopedic surgeon William Comai, D.O. “The exciting thing about having robotic surgery is that, as the technology progresses, we’ll be able to do better and better surgeries.”
The detailed anatomical view generated by a CT scan yield greater patient satisfaction in the long run, said Paul Aschmetat, D.O., the third member of Oaklawn’s board-certified orthopedics team. Since 2019, Aschmetat’s work with the robotic system has focused on hip procedures.
“This then can be fine-tuned intra-operatively to re-establish individual anatomy, including soft-tissue balancing and restoring leg lengths down to the millimeter,” he said.
Even for more difficult cases, using the robotic system optimizes total hip-replacement outcomes, Aschmetat said.
“I am confident that my patients will be happy with the end result of the procedure” when using the robotic system, he added.
Gregg Beeg, Oaklawn’s president and CEO, said the robotic system continues to play an important role for the hospital and its patients.
“We are proud to have been the first hospital in this region to use this highly advanced technology,” Beeg said. “Having this available for our patients is another demonstration of our commitment to the communities we serve.”
Oaklawn’s orthopedic services are based at the Marshall Specialty Clinic at 203 Winston Drive in Marshall. The office may be contacted at (269) 789-4380. More information about Oaklawn’s surgical team is available at oaklawnhospital.org/ortho.