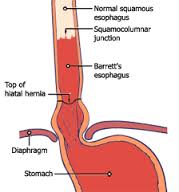
Barrett’s Esophagus
What is Barrett’s esophagus?
Barrett’s esophagus is a change in the lining of the esophagus caused by
chronic reflux of acid from the stomach. After years of acid splashing on the end
of the esophagus, the tissue may start to look like tissue from the intestine
instead of normal esophagus tissue.
What causes Barrett’s esophagus?
Barrett’s esophagus is caused by severe and chronic reflux of acid into the
esophagus. It is unclear why some patients with reflux develop Barrett’s
esophagus whereas others do not. Recently, a number of risk factors have been
defined for the development of Barrett’s esophagus:
- Early age at onset of reflux symptoms
- Long duration of reflux symptoms
- The presence of reflux symptoms at night
Patient’s at greatest risk of developing Barrett’s are white males over age 50 with a history of chronic heartburn.
What are the symptoms of Barrett’s esophagus?
The symptoms of Barrett’s esophagus are no different than the symptoms of uncomplicated gastroesophageal reflux disease. GERD. These include a burning sensation beneath the chest (heartburn) as well as acid regurgitation. These symptoms often resolve with medications that decrease acid in the stomach. Difficulty swallowing may also be seen in the setting of Barrett’s esophagus. This is a symptom that requires immediate attention.
How is Barrett’s esophagus diagnosed?
The diagnosis of Barrett’s esophagus is confirmed with a test called an EGD (Esophagogastroduodenoscopy). This involved inserting a small lighted tube (endoscope) through the throat and into the esophagus to look for a change in the lining of the esophagus characteristic of Barrett’s esophagus. While the appearance of the esophagus may suggest Barrett’s esophagus, the diagnosis can only be confirmed with small samples of tissue (biopsies) obtained through the endoscope. Biopsies can be taken without producing pain. X-rays cannot accurately detect Barrett’s esophagus.
How is Barrett’s esophagus treated?
The treatment is similar to the treatment of gastroesophageal reflux (GERD), namely, lifestyle changes in conjunction with the use of medications that will decrease acid production by the stomach. Patients with Barrett’s esophagus typically need very potent medications known as proton pump inhibitors to reduce acid. Examples of these medications are omeprazole (Prilosec), lansoprazole (Prevacid), esomeprazole (Nexium), pantoprazole (Protonix), and rabeprazole (Aciphex). These medications are typically taken with water 30 minutes to 1 hour before breakfast once a day or, on occasion, before breakfast and dinner.
Complications of Barrett’s esophagus.
Barrett’s esophagus is a precancerous lesion that may lead to the development of cancer of the esophagus in some patients. The overall risk of developing cancer is approximately 0.5% each year. As such, the majority of patients with Barrett’s esophagus will never develop cancer. Cancer in Barrett’s esophagus develops through a sequence of changes in the esophagus known as dysplasia. Dysplasia can only be detected by endoscopic biopsies. All patients with Barrett’s esophagus should have surveillance biopsies (every 1-2 years after initial diagnosis) in an effort to detect cancer at an early and potentially curable stage.
Are there any new treatments for Barrett’s esophagus?
There is much work underway to develop a new and more effective treatment for Barrett’s esophagus. One such treatment is known as ablation therapy. The principle of this treatment is to damage the lining of the esophagus with either heat or laser light and have normal cells develop in a setting of decreased acid production. While this type of therapy holds great promise for the future, it is experimental and unproven at this time. Other new treatments are also under development.
References: Cleveland Clinic, http://www.clevelandclinic.org/gastro/barretts/patient