Preventing Osteoporosis
Osteoporosis is a condition where bone density decreases and results in an increased risk for fracture. Typically we think of osteoporosis as a condition that effects the elderly, but a popular quote by Dr. Charles E. Dent says that “osteoporosis is a pediatric disease.” Being that we reach peak bone mass before age 30, if bone health isn’t emphasized during our earlier years, then we’re setting ourselves up for a disadvantage later in life.
Dietary Calcium
There are many ways to prevent osteoporosis, the most important of which is dietary calcium. The breakdown of calcium recommendations by age is as follows:
- Toddlers (1-4) – 700 mg/day
- Ages 4-8 – 1000 mg/day
- Ages 9-18 – 1300 mg/day
- Ages 19-70 – 1000 mg/day
- Ages 70+ – 1200 mg/day
Tip of the Day: When reading nutrition information, take the % RDA calcium on a product and add a zero. That is approximately equivalent to the milligrams of calcium. For example, if something contains 15% RDA then it is approximately 150 mg.
Calcium Source 1 = Dairy
Each serving of dairy (1 cup of milk, 1 ounce of cheese, 1 cup of yogurt) supplies approximately 300 mg of calcium, so reaching the above targets should be easy when following a healthy diet.
Dairy Guidelines for Children
- In most cases, children who are 12 months old and not breastfeeding should transition from formula to vitamin D whole cow’s milk.
- Low lactose and lactose free vitamin D milk are also options for toddlers with lactose intolerance.
- If toddlers cannot tolerate cow’s milk or the family chooses a non-dairy option, calcium-fortified soy milk is the best alternative given its supply of protein, calcium and other nutrients.
- It’s a good idea to avoid fat free or low fat options because fats are instrumental for brain development.
- In most cases, at age 2, it is appropriate to decrease milk fat intake by switching to low fat or fat free milk (low lactose and lactose free options are appropriate).
- Avoid or limit chocolate milk and sweetened rice milk, soy milk and almond milk.
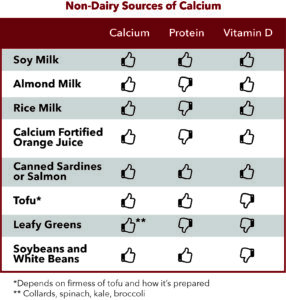
Calcium Source 2 = Non-Dairy
If you’re someone who limits or avoids dairy altogether, there are many good non-dairy sources of calcium that you can choose from. The table below outlines some of your best options, while also giving you an idea of whether or not these choices are good sources of protein and vitamin D.
The Vitamin D and Calcium Connection
Vitamin D is important for many reasons, but it’s essential when it comes to calcium because it helps with absorption. Getting your daily intake of calcium isn’t going to make much of a difference if your body doesn’t have what it needs to absorb it! If you’re deficient in vitamin D, you might experience fatigue, depression, and muscle and joint pain. Vitamin D recommendations are as follows:
- Breastfed infants – A vitamin D supplement supplying 400 IU (international units)/day is recommended.
- Formula fed infants and toddlers – If drinking vitamin D cow’s milk after age 1, your child should get adequate vitamin D without additional supplementation.
- Ages 1-70 – 600 IU/day
- 70+ – 800 IU/day
Other Ways to Prevent Osteoporosis
In addition to making sure you’re getting your daily dose of calcium and vitamin D, there are other steps you can take to prevent osteoporosis. Some of the most common include:
- Incorporate weight bearing exercise – Resistance training helps prevent osteoporosis because it strengthens muscle and builds bone, and increasing bone density has been shown to reduce fractures. So when you see the recommendation to get 30 minutes of exercise per day, think beyond cardio and add some lifting into your routine.
- Avoid smoking – This is especially important in the teen years and young adulthood because this is when peak bone mass is achieved. What this means is that if you don’t build bone during this time, then you’re not going to later. Studies have shown a direct connection between tobacco use and decreased bone density. As a result, smoking has been shown to increase the risk of fractures while also negatively impacting the fractured bone’s ability to heal.
- Limit alcohol – The main reasons why alcohol increases the risk of osteoporosis is because it negatively impacts the body’s balance of calcium AND it also interferes with the body’s production of vitamin D. Excessive alcohol consumption means that you’re taking a double hit – not only is calcium production disrupted, but your body’s ability to absorb it is impacted as well. Not to mention, alcohol impacts balance, which leads to an increased fall risk. Since your bones will be weakened, if you do happen to fall, it’s likely to result in a fracture. At maximum, adults should aim to limit alcohol intake to 2 drinks or less per day.
As always, if you have questions about osteoporosis, strike up a conversation with your primary care provider.